
Why Bottom-Up not Top-Down May Work for Mental Health!
Today is World Mental Health Day. Perhaps we should rename this as “The Role of the Nervous System World Mental Health Day.” Here is what I have learned through my own mental health healing journey.
When I was in my 20s and started having occasional panic attacks, I went to a psychologist and underwent what for many years was the go-to therapy for such issues: Cognitive Behavioral Therapy (CBT). In other words, we explored things from the top down—my thoughts were creating these bodily issues, so the answer was to change my thoughts. To this day, most therapists still offer CBT as a preferred form of treatment, and it does help develop skills to change thoughts to manage stress helping many to have a happier, so-called normal life. But we have learned a lot about how the body and mind interact through the nervous system recently. And many therapists and coaches, including me, are now incorporating this new knowledge in understanding and helping clients get to the root causes of these mental health issues. In other words, in many cases, there may be nothing wrong with our brains. It may be about our dysregulated nervous systems.
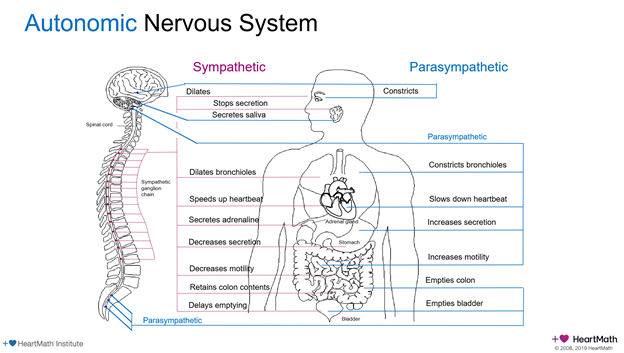
Autonomic Nervous System Then and Now
The autonomic nervous system, including the all-important Vagus Nerve complex, is a very large set of nerves in a two-way superhighway with more information going up from the body to the brain than down from the brain to the body. This major player in our physical and mental health is known as the wandering nerve because it affects and is affected by so many systems of the body from the smile on your face to the tone of voice, from the health of the physical and emotional heart to the state of your gut. And of course, it connects with nerves throughout the body as well. So as far as dealing with mental health issues such as anxiety, which I was experiencing, and chronic body issues created from the stress hormones being pumped through my system from the anxiety, changing my thoughts would help somewhat, but not completely. I learned it was more important to change what I was feeling in my heart, my gut, and other parts of my body connected to my nervous system. To heal, I discovered I had to change my physiology. My journey became a search for the reasons why “feeling unsafe in what I perceived was an increasingly unsafe world” (Jan Winhall) was manifesting itself as dis-ease. My body was indeed keeping the score, as Bessel Van der Kolk, MD, wrote in his best-selling book on the effects of trauma, The Body Keeps the Score.

The Role of the Vagus Nerve in Healing
Eight years ago, I started investigating the role of the vagus nerve in what was going on in my body and my mind, as well as the minds and bodies of my clients. I did so because I discovered no matter how much I changed their diet or mine, supplements, toxic exposures, exercise, sleep habits and other lifestyle factors, we were still not healing 100%. There were a few pivotal books and theories that have really changed the way I approach healing. One was The Last Best Cure by Donna Jackson Nakasawa, her own inspirational story of her “quest to awaken healing parts of my brain and get back my body, my joy and my life.” What worked for her was incorporating nervous system regulation practices daily like meditation and yoga. I also have read many books from the yoga tradition which focused on yoga for vagal toning. Most of my yoga classes include these practices including Mudras, mantras, and breath practices. Click here to sign up for my weekly live classes.
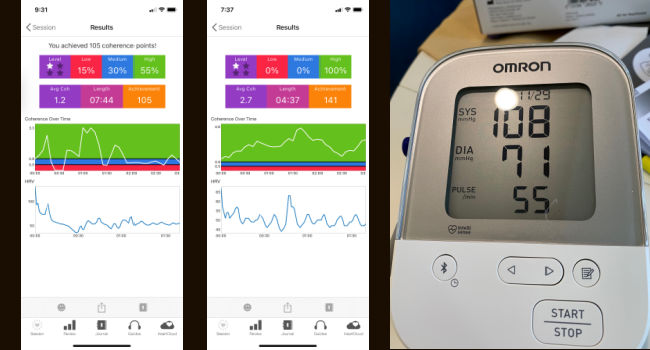
The HeartMath® trainings and books that I have immersed myself in during the past two years introduced me to a system of tools for self-regulation and co-regulation of the nervous system and skills for developing coherence between the heart, brain, endocrine, respiratory and other systems. These tools are so simple, yet profound when it comes to healing the nervous system. They also help create a feeling of safety and being socially connected through co-regulating.
New Tools for Healing: The Polyvagal Theory
I have also discovered the work of Dr. Stephen Porges and the Polyvagal theory. I am currently taking his online course. I have also read and implemented the work from Polyvagal Therapist Deb Dana from her book The Polyvagal Theory in Therapy. These tools are aimed at creating a feeling of safety within my clients and students by empowering them to shift their own nervous systems from one state to another. What is most interesting to me about the Polyvagal theory is that it explains three states of the nervous system: 1) why a person might get stuck in the fight or flight system known as the sympathetic branch of the vagus nerve; 2) why a person might shut down and become unable to deal with life when their dorsal branch of the parasympathetic system kicks in as a form of protection; 3) and how our need to feel safe and social is created through the ventral vagal system. Each of these systems has been around a long time in human evolution and is considered autonomic. The oldest system is the Dorsal shutdown branch. The Polyvagal theory while acknowledging that these systems turn on without our control in perceived dangers, also gives hope to clients that they can learn to shift from one state to another through lots of practice, tools, and a very compassionate, knowledgeable therapist or coach. In other words, the nervous system can become a tool for healing.
“We All Have to Settle Our Nervous Systems” according to Jan Winhall who addresses Trauma and Addiction through the Polyvagal lens.
Psychotherapist Jan Winhall, MSW, FOT, who wrote Treating Trauma and Addiction with the Felt Sense Polyvagal Model says “we all have to settle our nervous systems. Addicted or not, we are often emotionally dysregulated which affects our thinking and responding to the problem… We are all wired to survive any way we can. Polyvagal theory teaches us to pay attention to our bodies’ awareness of safety/danger and to notice and honor our autonomic nervous system’s bodily response.”

Simply stated, we need to spend more time listening to what is going on in our bodies to sense when and how we feel safe or not safe. When we are not feeling safe, rather than numbing those feelings through medicines or trying to feel better through addictive behaviors “that help, but hurt us” according to Ms. Winhall, we can learn how to safely explore them and move through them and over time, re-regulate our nervous systems and get back to living from a safe and social place.
As I learn more I will share more. But the bottom line is that if you are struggling with your mental and physical health, you might want to understand the state of your nervous system and begin to explore ways to feel safe in your body again.
Namaste,
Andrea



